
Sleep Disruption: The Silent Saboteur of Memory and Cognitive Function
Chronic sleep disruption, manifesting as insufficient duration, poor quality, or irregular sleep patterns, profoundly impacts the brain’s ability to form, consolidate, and retrieve memories, alongside a cascade of other cognitive functions. This intricate relationship between sleep and cognition is not merely correlational; it is mechanistically driven, involving critical neurobiological processes that occur primarily during sleep. Understanding these mechanisms is vital for recognizing the pervasive and often underestimated consequences of sleep deprivation on our mental acuity, decision-making capabilities, and overall cognitive health. The brain, during sleep, is not inert; it is actively engaged in crucial restorative and organizational tasks that are indispensable for optimal functioning when awake. Without adequate and high-quality sleep, these processes are compromised, leading to tangible deficits in memory, attention, executive functions, and problem-solving abilities.
The Consolidation of Memories: A Sleep-Dependent Orchestration
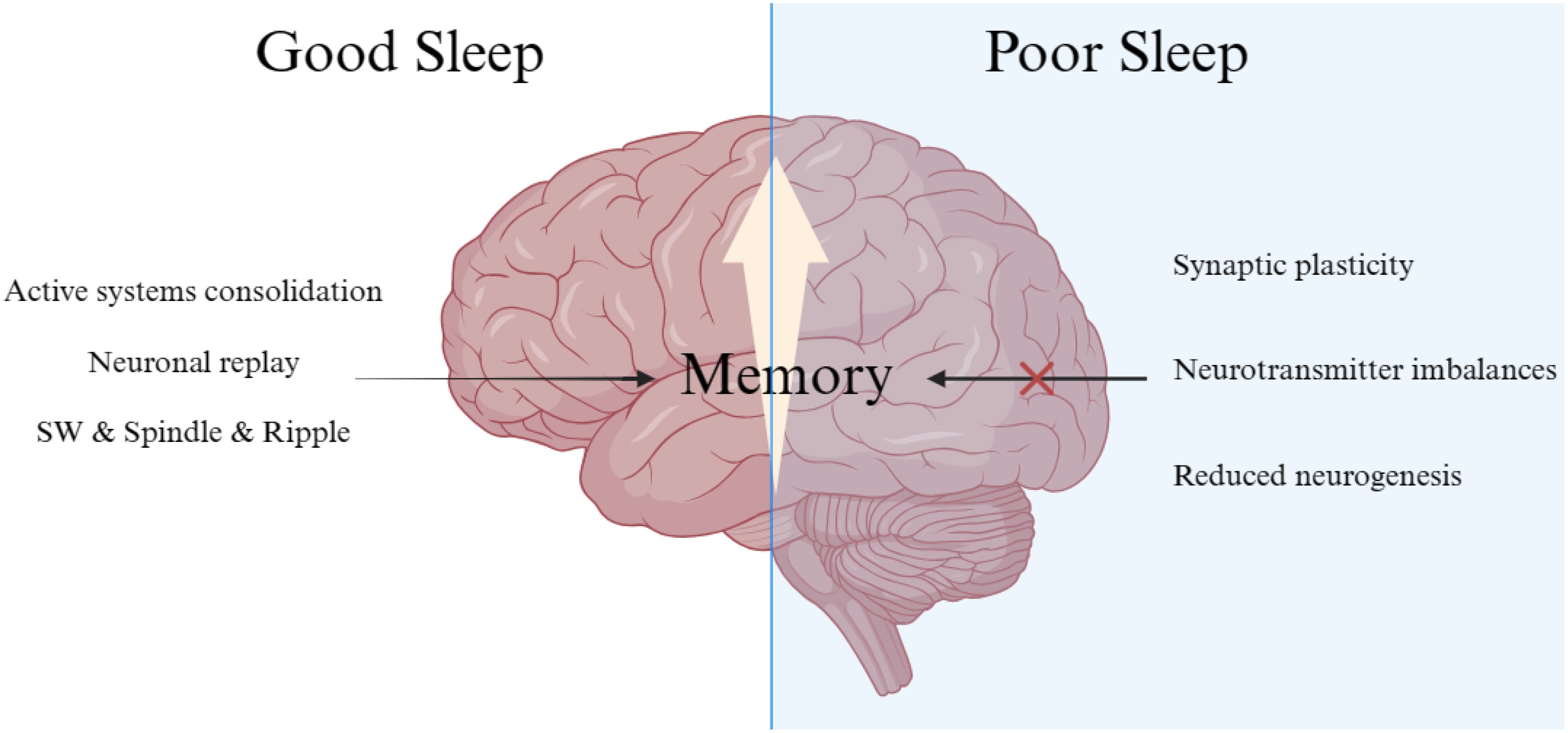
Memory formation is a multi-stage process involving encoding, consolidation, and retrieval. Sleep plays a paramount role in memory consolidation, the process by which newly acquired, fragile memories are stabilized and strengthened for long-term storage. This occurs primarily during specific sleep stages, most notably slow-wave sleep (SWS) and rapid eye movement (REM) sleep. During SWS, characterized by slow, high-amplitude brain waves, the hippocampus, a brain region critical for forming new episodic and semantic memories, appears to "replay" recent neural activity patterns. This replay is thought to facilitate the transfer of information from the hippocampus to the neocortex for more permanent storage. Disruptions to SWS, such as those experienced in insomnia or sleep apnea, directly impair this crucial hippocampal-neocortical dialogue, leading to poorer recall of newly learned information. REM sleep, on the other hand, is heavily implicated in consolidating procedural memories (skills and habits) and emotional memories. The unique neurochemical environment and brain activity patterns during REM sleep, including increased acetylcholine and decreased norepinephrine, are believed to foster synaptic plasticity and integrate new experiences with existing knowledge networks. Insufficient REM sleep, often a consequence of fragmented sleep or certain sleep disorders, can therefore hinder the acquisition of new skills and the processing of emotional experiences.
The Role of Sleep Spindles and Sharp-Wave Ripples
Beyond the broader sleep stages, specific neurophysiological events occurring during sleep are directly linked to memory consolidation. Sleep spindles, transient bursts of oscillatory brain activity primarily observed in stage 2 NREM sleep, are strongly associated with the consolidation of declarative memories (facts and events). These spindles are thought to facilitate synaptic plasticity and to synchronize neuronal firing, allowing for the integration of new information. Studies have shown a positive correlation between the density and duration of sleep spindles and subsequent memory performance. Similarly, sharp-wave ripples (SWRs), brief, high-frequency oscillations originating in the hippocampus, are another critical component of memory consolidation during SWS. SWRs are believed to be the neural substrate for the aforementioned hippocampal replay, driving the transfer of memories to the neocortex. Disrupted sleep often leads to a reduction in the occurrence and quality of both sleep spindles and SWRs, directly compromising the brain’s ability to solidify memories.
Impact on Encoding and Retrieval: The Awake Brain’s Suffering
While consolidation is heavily sleep-dependent, sleep disruption also negatively affects the earlier stage of memory formation: encoding. During wakefulness, effective encoding relies on sustained attention, working memory capacity, and the ability to efficiently process new information. Sleep deprivation significantly impairs attention, leading to distractibility and difficulty focusing on incoming stimuli. This reduced attentional focus means that less information is effectively registered by the brain in the first place, making subsequent consolidation and retrieval more challenging. Working memory, the temporary storage and manipulation of information, is also severely compromised by sleep loss. This deficit hinders the ability to hold and process multiple pieces of information simultaneously, further degrading encoding efficiency. Furthermore, sleep deprivation impairs the ability to retrieve existing memories. Even well-established memories can become harder to access when the brain is in a sleep-deprived state. This may be due to alterations in the neural networks involved in memory recall, or a general reduction in the brain’s processing speed and efficiency. The subjective experience of this can range from mild forgetfulness to more significant difficulties in recalling names, facts, or recent events.
Executive Functions: The Higher-Order Cognitive Toll
Beyond memory, disrupted sleep has a profound and detrimental impact on executive functions, a suite of higher-order cognitive processes that enable goal-directed behavior, planning, and self-regulation. These functions are largely mediated by the prefrontal cortex, a brain region particularly vulnerable to the effects of sleep deprivation. Key executive functions affected include:
- Decision-Making: Sleep deprivation impairs the ability to make sound and rational decisions. This is often characterized by an increased propensity for risk-taking, impaired judgment, and difficulty in evaluating potential consequences. The brain’s reward system becomes hyperactive, while regions responsible for impulse control and executive control are less effective, leading to poor choices.
- Problem-Solving: The ability to analyze situations, generate solutions, and adapt strategies is severely hampered by insufficient sleep. Sleep-deprived individuals often exhibit rigid thinking, a reduced capacity for abstract reasoning, and difficulty in generating novel approaches to problems.
- Planning and Organization: The capacity to set goals, devise steps to achieve them, and manage time effectively is diminished. Individuals may struggle with task initiation, procrastination, and maintaining a structured approach to daily activities.
- Cognitive Flexibility: The ability to switch between tasks, adapt to changing circumstances, and consider different perspectives is compromised. Sleep deprivation leads to mental inflexibility, making it harder to adjust to new information or shift focus when needed.
- Working Memory: As previously mentioned, working memory deficits directly impede executive functions by limiting the capacity to hold and manipulate information relevant to ongoing tasks.
Attention and Vigilance: The Foundation of Cognitive Performance
Attention, the cognitive process of selectively concentrating on one aspect of the environment while ignoring others, is fundamental to nearly all cognitive operations. Sleep disruption unequivocally degrades attentional capacity. This manifests as:
- Reduced Sustained Attention: The ability to maintain focus over extended periods diminishes significantly. This leads to frequent mind-wandering and difficulty completing tasks that require prolonged concentration.
- Increased Lapses in Attention: Brief, involuntary breaks in attention become more frequent and pronounced, increasing the likelihood of errors and accidents. These lapses can be particularly dangerous in tasks requiring vigilance, such as driving or operating machinery.
- Impaired Selective Attention: The ability to filter out irrelevant stimuli and focus on pertinent information is compromised. This can lead to increased distractibility and a struggle to prioritize information.
The impact on vigilance, the state of being alert and ready to respond to stimuli, is particularly critical in safety-sensitive occupations. Sleep-deprived individuals exhibit a marked decline in vigilance, leading to an increased risk of errors and accidents.
Neurobiological Underpinnings: Neuronal Communication and Plasticity
At a cellular and molecular level, sleep disruption leads to widespread alterations in neuronal function and plasticity. Adenosine, a neuromodulator that accumulates in the brain during wakefulness and promotes sleep, plays a crucial role. During sleep, adenosine levels are reduced through metabolic processes, facilitating wakefulness. However, chronic sleep deprivation leads to persistently high adenosine levels, which can interfere with neurotransmitter systems, including dopamine and norepinephrine, critical for attention and arousal. Furthermore, sleep is essential for synaptic homeostasis, a process that involves the weakening of some synapses and strengthening of others, thereby preventing neural circuits from becoming saturated. Disruptions to sleep interfere with these homeostatic mechanisms, potentially leading to maladaptive synaptic changes that impair cognitive processing. Neuroinflammation, an increase in inflammatory markers within the brain, is also increasingly linked to sleep disruption and cognitive decline. Chronic sleep deprivation can exacerbate neuroinflammatory processes, which can damage neurons and impair synaptic function, contributing to memory and thinking problems.
The Gut-Brain Axis: An Emerging Connection
Recent research has highlighted the intricate connection between the gut microbiome and brain function, often referred to as the gut-brain axis. Disruptions in sleep can alter the composition and function of the gut microbiota, which in turn can influence brain health and cognition. Changes in gut bacteria can lead to altered production of neurotransmitters and metabolites that can impact mood, cognition, and inflammation. Emerging evidence suggests that sleep deprivation can negatively affect the gut microbiome, potentially contributing to the cognitive deficits observed in sleep-disordered individuals. This bidirectional relationship underscores the systemic impact of poor sleep on overall well-being, extending beyond the brain to influence other physiological systems.
Consequences of Chronic Sleep Disruption: A Widespread Impact
The persistent impact of disrupted sleep on memory and cognition can have far-reaching consequences for individuals and society. In academic settings, students struggling with sleep deprivation may experience declining grades and difficulty learning new material. In the workplace, impaired decision-making, reduced productivity, and increased errors can have significant economic implications. On a personal level, individuals may experience frustration, social withdrawal, and a diminished quality of life due to ongoing cognitive challenges. Furthermore, chronic sleep disruption is increasingly recognized as a risk factor for the development of neurodegenerative diseases, including Alzheimer’s disease, where impaired memory and cognitive decline are hallmark symptoms. The accumulation of beta-amyloid, a protein implicated in Alzheimer’s, appears to be exacerbated by sleep deprivation, suggesting a potential mechanistic link between sleep health and long-term brain integrity.
Conclusion: Prioritizing Sleep for Cognitive Resilience
The evidence overwhelmingly demonstrates that disrupted sleep is not a benign inconvenience but a significant threat to cognitive function. The intricate neurobiological processes that underpin memory formation, consolidation, and retrieval, as well as executive functions and attention, are profoundly dependent on adequate and quality sleep. Recognizing the pervasive impact of sleep disruption is the first step towards addressing this critical public health issue. Strategies to improve sleep hygiene, manage sleep disorders, and promote a societal understanding of sleep’s vital role in cognitive health are essential for fostering individual and collective cognitive resilience. Prioritizing sleep is not merely a matter of personal well-being; it is a fundamental investment in our cognitive capacity and long-term brain health.